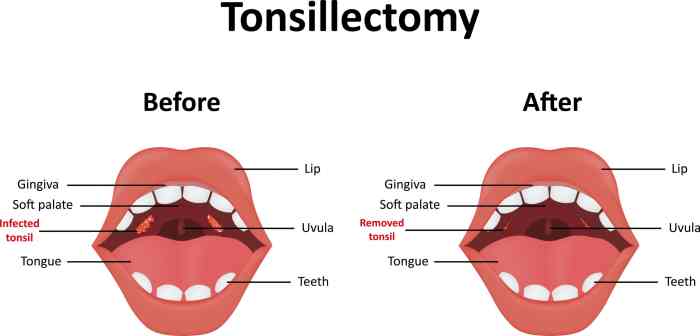
 It is very common in the US and around the world to remove the tonsils of children children.
It is very common in the US and around the world to remove the tonsils of children children.
Tonsillectomy is the second most common pediatric surgical procedure. These days, ear, nose and throat specialists perform about half as many tonsillectomies as they did in the 1950s and ’60s. Tonsillectomy is generally performed because of repeat occurrences of tonsillitis. Tonsillitis is an infection in the throat that starts with your tonsils. These types of sore throats are usually severe and fever can occur. Many doctors believe that a tonsillectomy can help prevent frequent sore throats and ear infections.
However a new study published in June 2018 in the Journal of the American Medical Association Otolaryngology Head and Neck Surgery,suggests that the surgery may have long-term risks that in some cases outweigh any short-time benefits.
This is the first study to look at long-term risks which compared 60,667 Danish children under 9 who had tonsillectomies, adenoidectomies or both with 1.1 million who had not had the surgeries. They were born between 1979 and 1999, and researchers followed their health for up to 30 years.
They found that tonsillectomy was associated with almost triple the relative risk of diseases of the upper respiratory tract. These included asthma, influenza, pneumonia and chronic obstructive pulmonary disorder or COPD, the umbrella term for diseases like chronic bronchitis and emphysema. Adenoidectomy was associated with about double the relative risk of obstructive pulmonary disorder, upper respiratory tract diseases and conjunctivitis.
The surgery has some short-term benefits in cases of abnormal breathing, sinusitis and ear infections, but the long-term risks for those conditions were either significantly higher after surgery or not significantly different.
The researchers wrote: “Given that tonsils and adenoids are part of the lymphatic system and play a key role both in normal development of the immune system and in pathogen screening during childhood and early life, it is not surprising that their removal may impair pathogen detection and increase risk of later respiratory and infectious diseases.”
The researchers also found heightened susceptibility to 28 different types of disease, including parasitic infections, skin diseases and eye complaints – 78 percent of these were experienced more commonly in people who had these surgeries. These are unrelated to the airways and suggest there is some knock-on impact on the immune system from the loss of your tonsils or from the repeated minor infections this brings – this may become even more pronounced as the population ages.
“Our results show increased risks for long-term diseases after surgery, support delaying tonsil and adenoid removal if possible, which could aid normal immune system development in childhood and reduce these possible later-life disease risks,” said lead author Dr Shaun Bayers, from the University of Melbourne.
I believe that none of our organs are unnecessary. Not only are tonsil and adenoid removals common, but also appendix and gall bladder removal. We need to look at the body as a whole when it comes to treatment. Definitely missing one organ will affect another. Please pay attention to detail and be aware of long-term risks if you consider organ removal. Especially when a small child is involved, please look into alternative treatments.
Source:
https://www.telegraph.co.uk/science/2018/06/07/having-tonsils-triples-risk-asthma-according-major-study/
http://www.greenmedinfo.com/blog/removing-childrens-tonsils-and-adenoids-increases-risk-28-diseases-study-finds